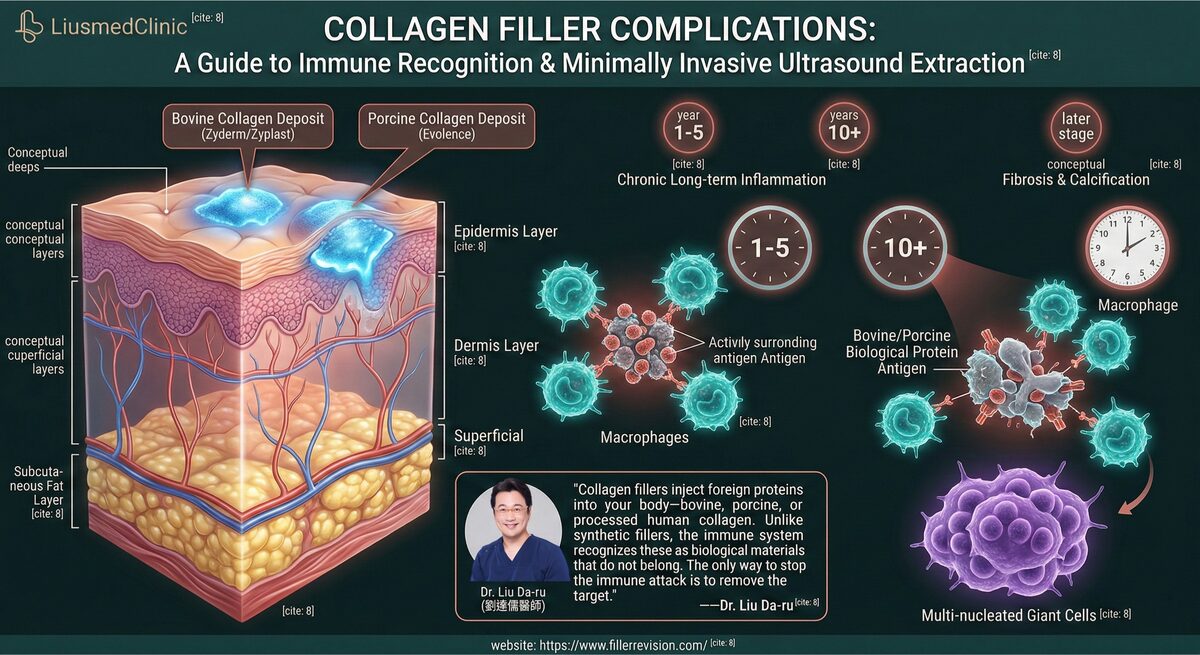
Our Core Technology
The gold standard for filler complication management · Minimally invasive · Visually guided
Why Choose Ultrasound-Guided Removal?
| Method | Visibility | Material Types | Invasiveness | Risk |
|---|---|---|---|---|
| Blind Dissolving | None (Blind) | HA Only | Injection only | Tissue atrophy / Incomplete removal |
| Surgical Excision | High (Open) | All Types | High (Large Incisions) | Scarring, Nerve damage |
| Ultrasound-Guided Pinhole | High (Real-time) | All (HA, Sculptra, Fat, PMMA) | Low (Pinhole) | Minimal |
Why Ultrasound Changes Everything
Real-time imaging transforms filler removal from guesswork into precision medicine
See What You're Treating
Ultrasound reveals whether filler is encapsulated, free-flowing, fragmented, or necrotic. Each pattern requires a completely different extraction strategy. Without imaging, doctors are guessing — and guessing leads to incomplete removal or tissue damage.
Protect Critical Structures
The face contains a dense network of nerves, arteries, and veins within millimeters of filler deposits. Real-time imaging lets us navigate around these structures with sub-millimeter precision, dramatically reducing the risk of nerve injury or vascular damage.
Verify Complete Removal
The most common reason for 'failed' filler removal is residual material left behind. With ultrasound, we confirm complete extraction before the procedure ends — you don't need to come back wondering why there's still a lump.
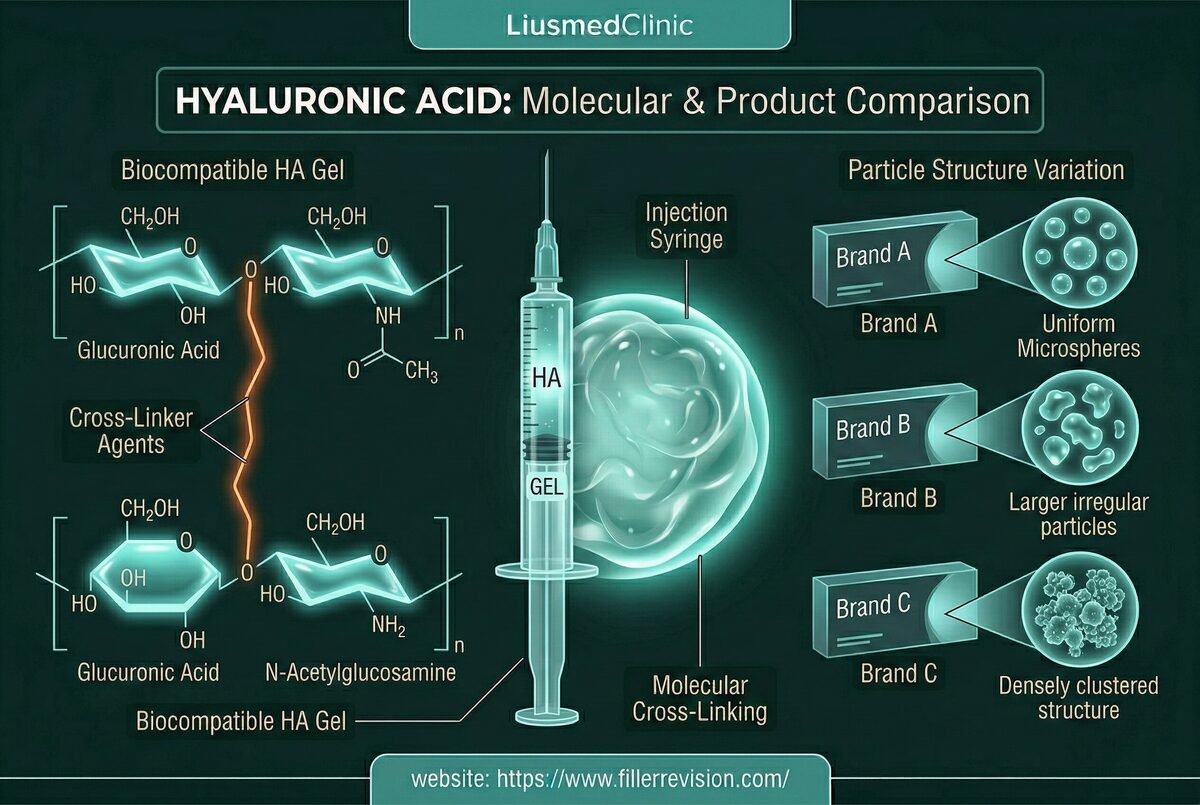
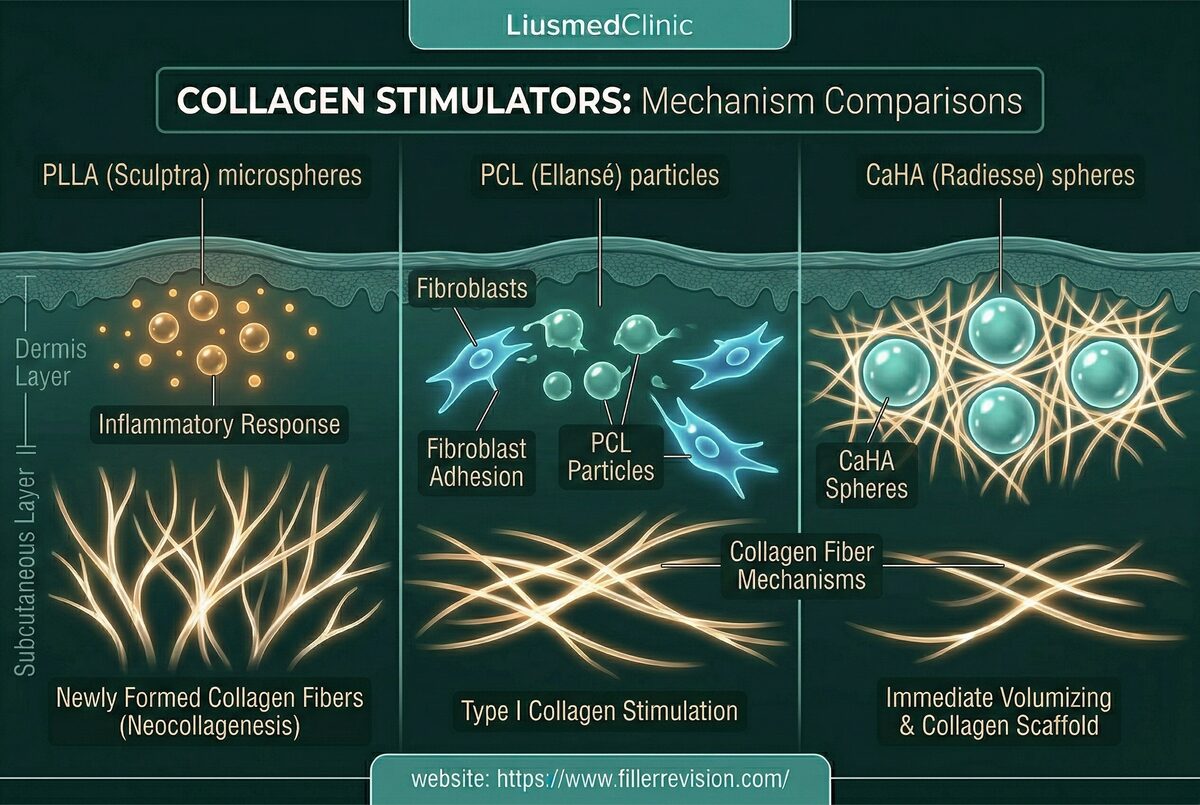
Material Classification Drives Treatment
HA, collagen stimulators, fat, silicone, and PMMA all look different on ultrasound. This classification determines the optimal extraction technique: enzyme flush for accessible HA, mechanical fragmentation for Sculptra nodules, progressive debulking for permanent fillers.
The Procedure
Four precision steps, from diagnosis to verified complete removal
1. Ultrasound Mapping
We use high-frequency ultrasound to map the exact depth, volume, and location of the filler material relative to blood vessels and nerves. This diagnostic phase identifies whether material is encapsulated, free-flowing, or fragmented — each requiring a different extraction strategy. The ultrasound also reveals any vascular compromise or tissue changes that affect our approach.
Different filler materials have distinct ultrasound signatures, allowing us to classify the problem before we begin.
2. Micro-Dissection
Under real-time ultrasound guidance, precision instruments create a safe dissection plane along tissue layers, pushing nerves, vessels, and other vital structures away from the filler/granuloma. This step ensures surrounding healthy tissue is protected during extraction. For encapsulated material, micro-dissection precisely defines the capsule boundary so we can extract it intact.
Working along anatomical planes under ultrasound visualization allows safe operation even millimeters from nerves and vessels.
3. Micro-Fragmentation
For solid materials or hard nodules, we use specialized energy or mechanical instruments to break the material into extractable pieces. The technique varies by material — collagen stimulators require different fragmentation than silicone or calcified fat. Throughout this step, ultrasound monitoring ensures we're targeting only foreign material.
This is where material-specific expertise matters most: each filler type has optimal fragmentation parameters.
4. Pinhole Extraction
Through a needle-sized entry point, the material is flushed and aspirated out. No scalpel, no stitches, minimal downtime. Real-time ultrasound confirms complete removal before we finish — you don't leave wondering if material was left behind. The entry point is typically 1-2mm, healing without visible scarring.
We verify extraction completeness with post-procedure ultrasound imaging, ensuring nothing is left behind.
By Symptom
Revision protocols classified by clinical presentation
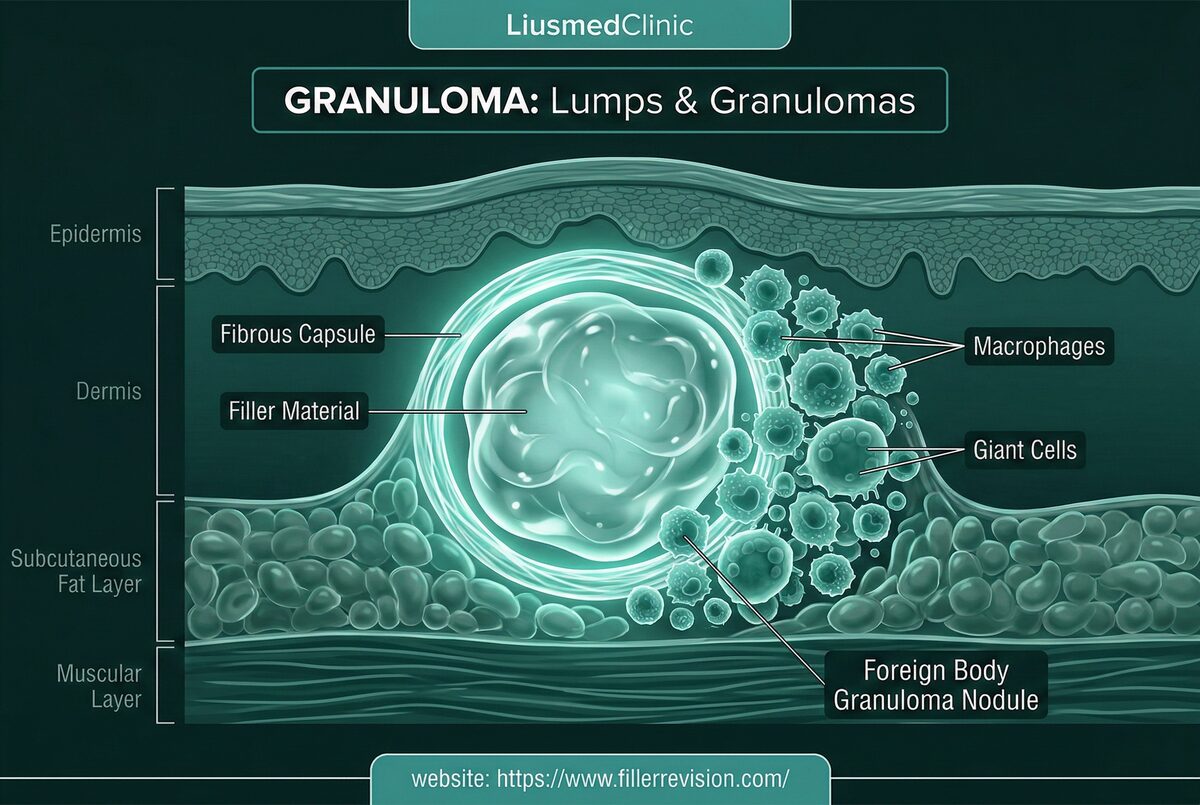
Lumps & Granulomas
Hardened immune reactions.
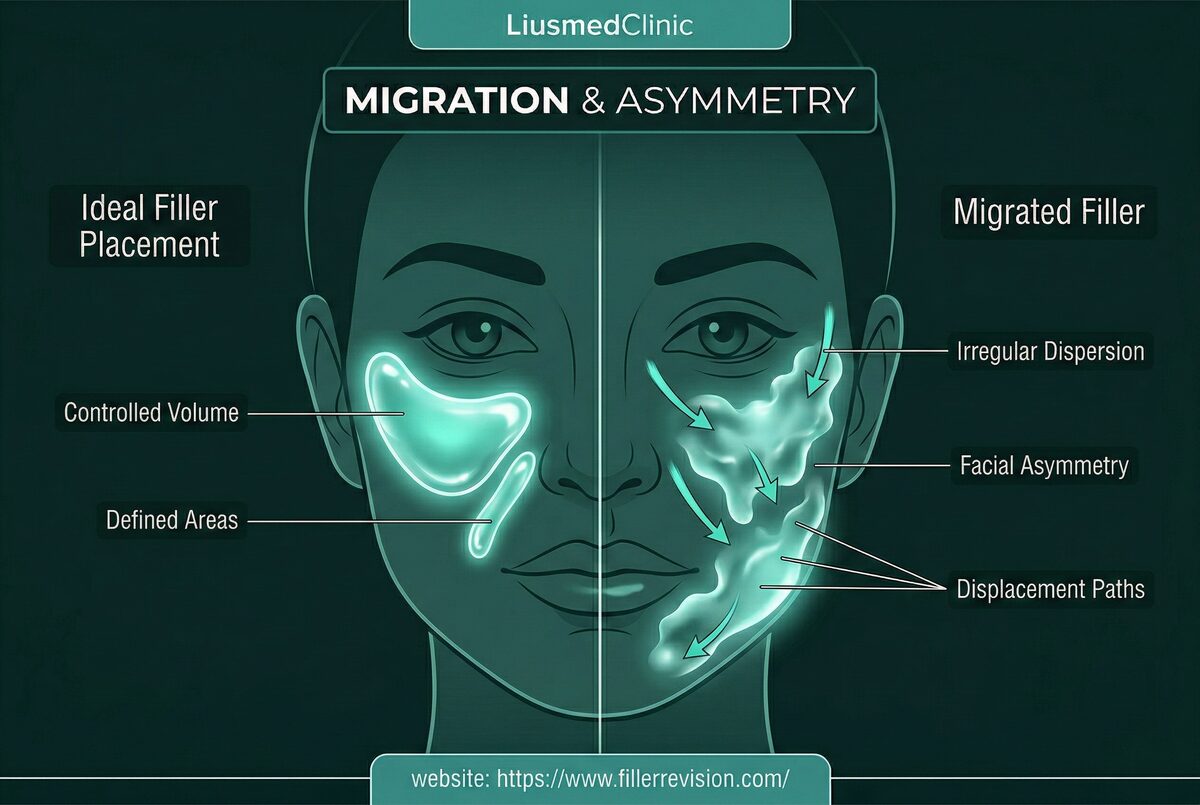
Migration & Asymmetry
Displaced material correction.
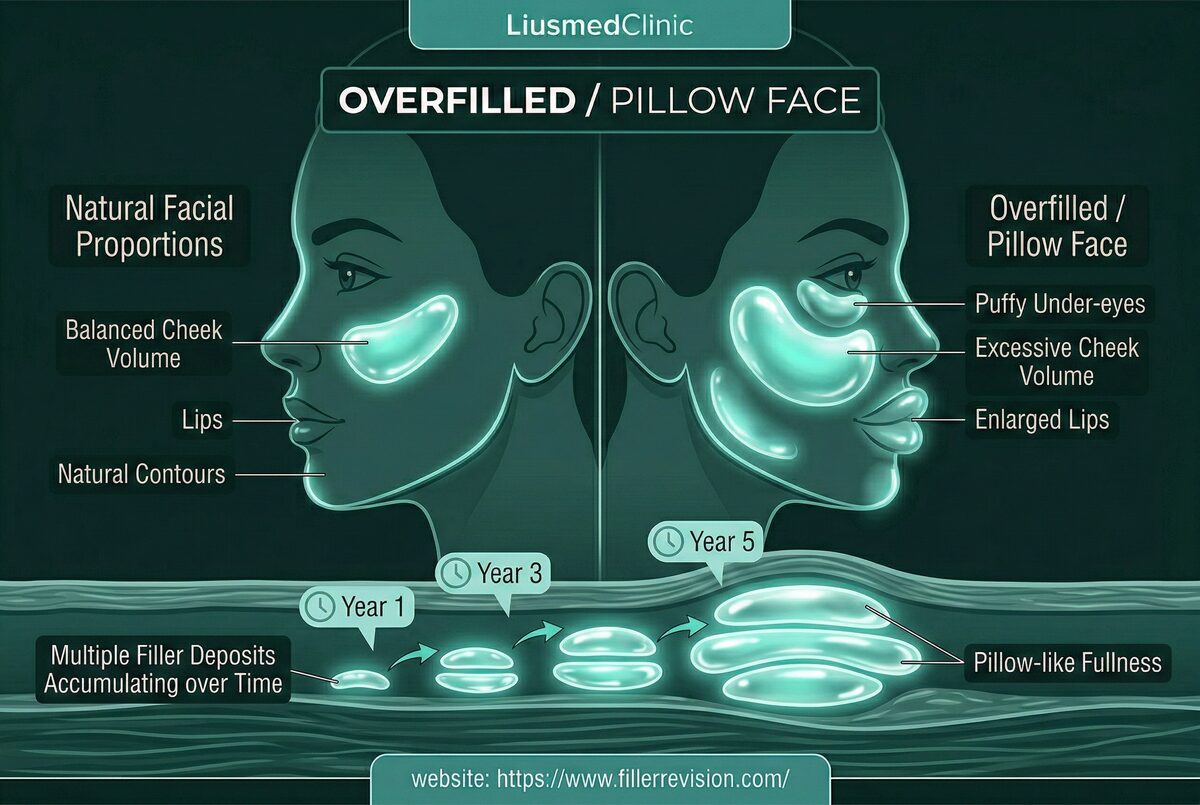
Overfilled Syndrome
Pillow face / Avatar nose.
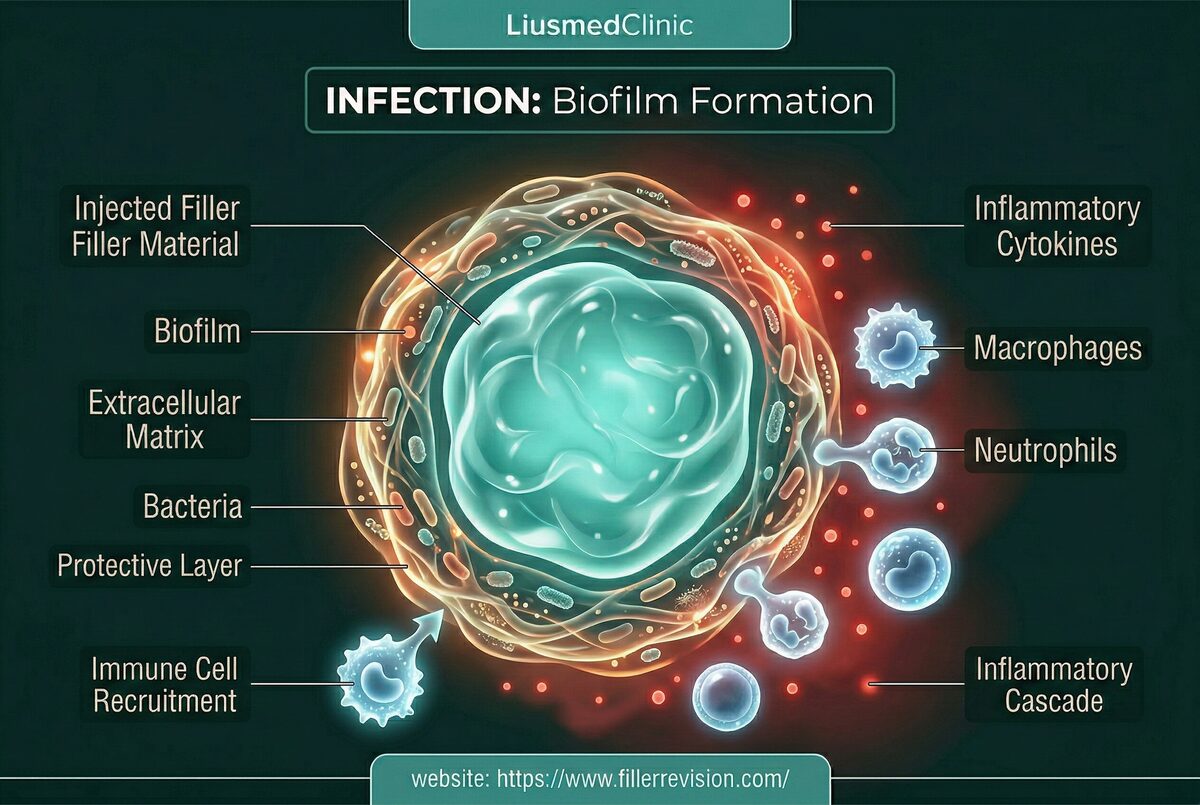
Infection & Biofilms
Chronic, recurrent swelling.
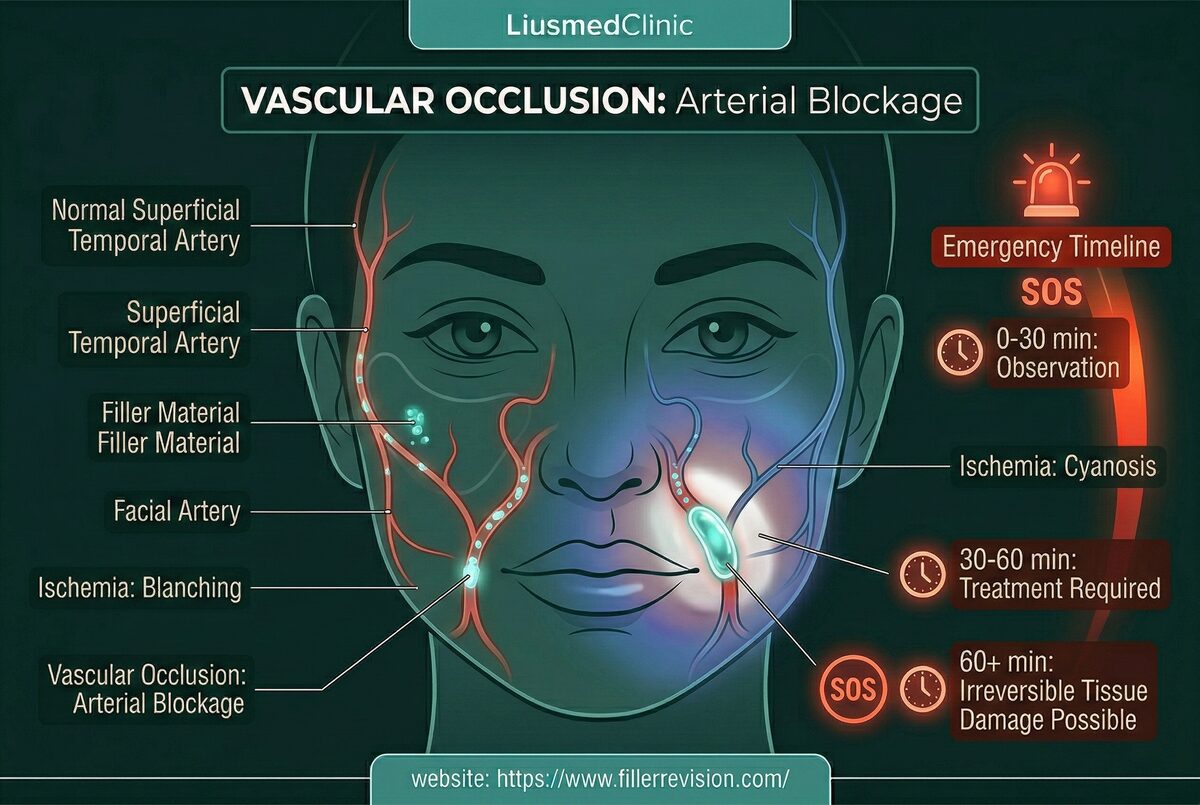
Vascular Occlusion
Post-occlusion recovery & scar repair.
By Material
Revision protocols classified by filler material type
Featured Poster
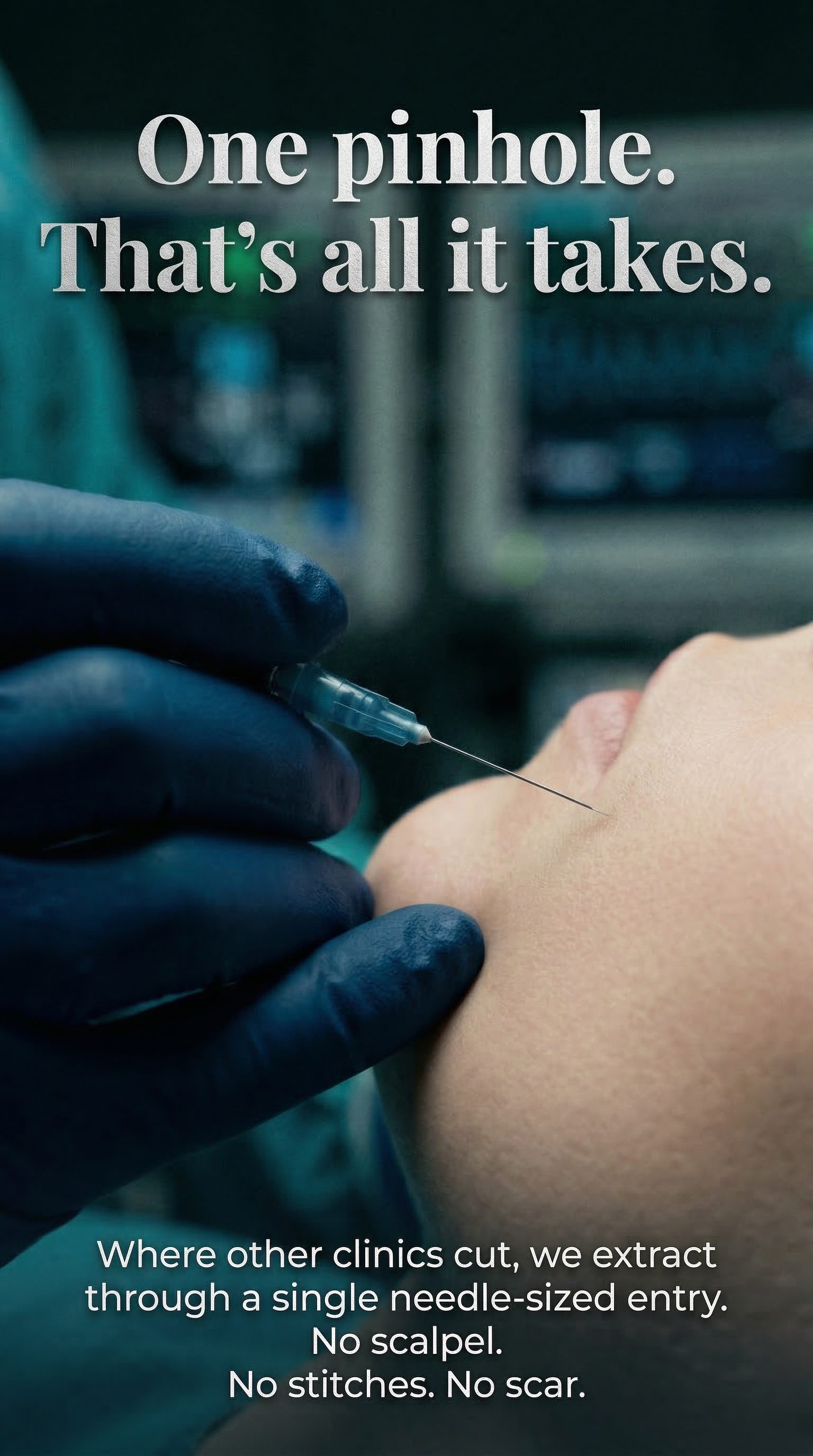
One pinhole. That's all it takes.
Where other clinics cut, we extract through a single needle-sized entry. No scalpel. No stitches. No scar.

Days 7–14. Back to a confident life.
A tiny pinhole, mild swelling, and bruising. No stitches, zero scars. By days 7–14, you're already back to normal life — minus that annoying lump.
Frequently Asked Questions
Most procedures take 30-90 minutes depending on the volume and type of material, the number of areas treated, and whether the filler is encapsulated. Complex cases with multiple filler types or extensive migration may require longer sessions.
We use local anesthesia for all procedures, so you'll feel pressure but not pain during the extraction. Most patients describe it as less uncomfortable than the original filler injection. Post-procedure soreness is mild and typically resolves within 2-3 days.
Most patients return to normal activities within 3-7 days. Expect mild swelling and possible bruising at the treatment site. We provide detailed aftercare instructions and a follow-up ultrasound to confirm complete removal. Strenuous exercise should be avoided for 1-2 weeks.
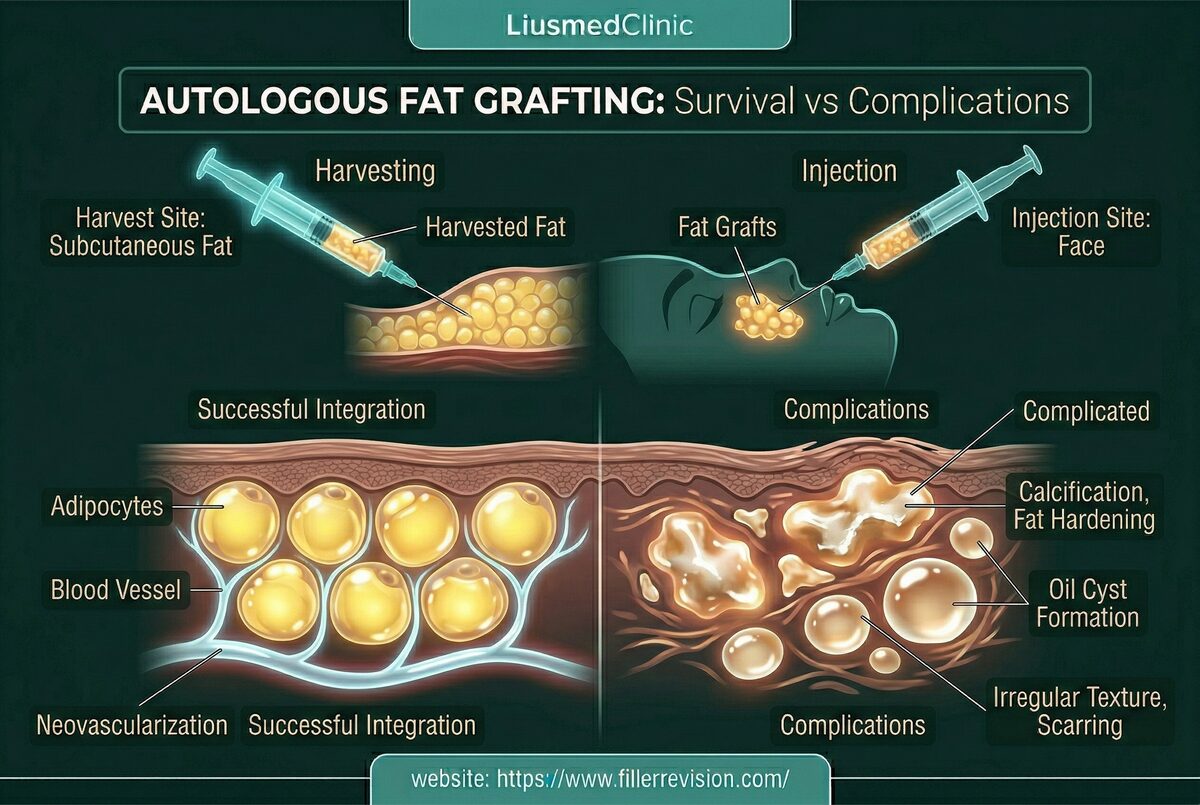
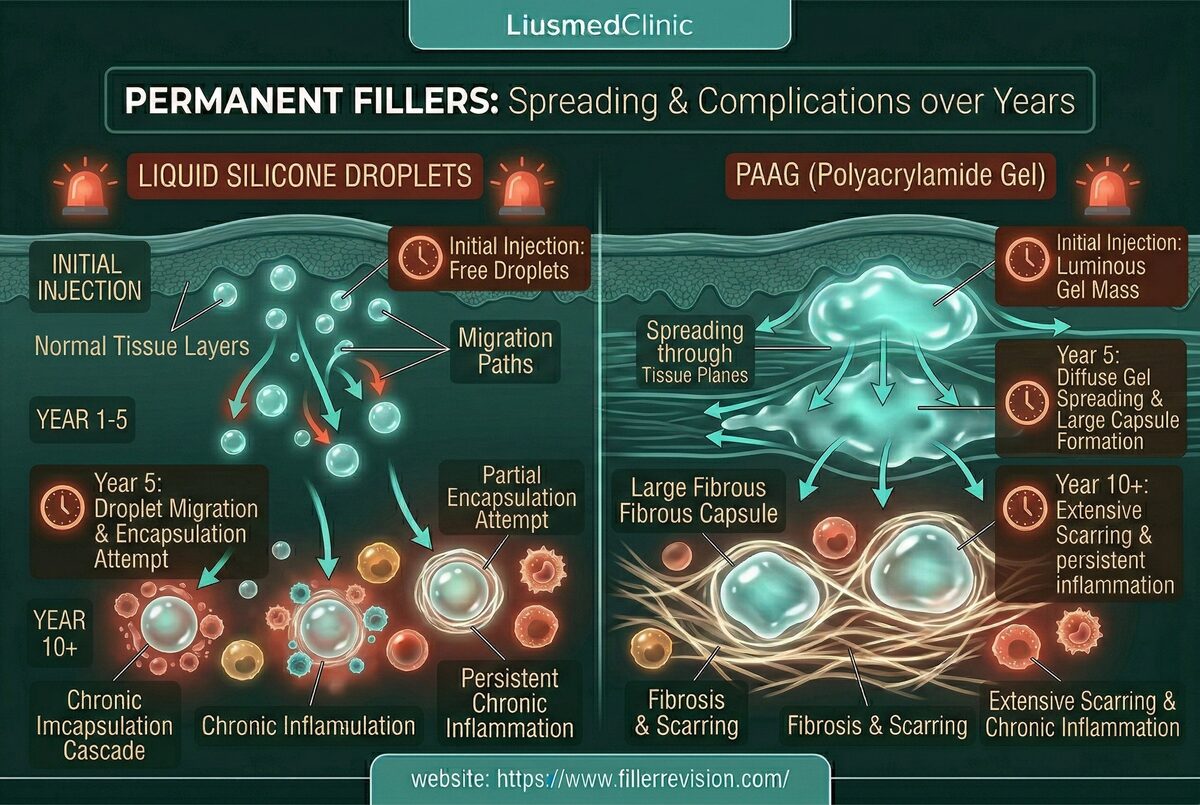
Yes. Our ultrasound-guided technique works on all injectable materials: hyaluronic acid (Juvederm, Restylane), collagen stimulators (Sculptra, Ellansé), calcium hydroxylapatite (Radiesse), fat grafting, silicone, PMMA, and other permanent fillers. The technique is adapted for each material type.
Over 95% of cases are resolved in a single session. Complex situations — such as extensive permanent filler deposits or multiple treatment areas — may require 2-3 staged sessions for optimal results and safety.
The entry point is approximately 1-2mm (needle-sized), which heals virtually invisible within weeks. Unlike surgical excision which requires incisions of 1-5cm, our pinhole technique leaves no visible scars. This is one of the key advantages over traditional surgical approaches.
Many patients come to us after being told their situation is hopeless. 'Untreatable' usually means the previous doctor didn't have the right tools. Blind injection techniques fail when capsules form around filler. Our ultrasound-guided approach physically removes encapsulated material — this is why it works when dissolving agents don't.
The information on this website is for educational purposes only and does not constitute medical advice. Individual results may vary depending on personal conditions; actual outcomes cannot be guaranteed. All medical procedures carry potential risks and complications. Please consult a qualified physician before making any treatment decisions.
Posted in the forum? We can help expedite your appointment.
Standard booking takes 3+ months. If you post your case in the FillerRescue forum first and then add LINE @liusmed with the required info, we’ll watch for earlier slots and help arrange your appointment as soon as possible.
In your LINE message, mention you posted in the FillerRescue forum.