Collagen Filler Complications
"I told my new dermatologist about the lumps and she said she's never even heard of Zyderm. Where do I go for something this old?" At FILLER REVISION, we hear this from patients whose collagen filler complications predate most modern practitioners' careers. Legacy collagen fillers from the 1980s-2000s are resurfacing as complications decades later. Bovine collagen (Zyderm, Zyplast), porcine collagen (Evolence), and human-derived products (CosmoDerm, CosmoPlast) were the original soft-tissue fillers. Although replaced by HA in modern practice, millions of patients still carry residual deposits. These products inject actual foreign protein into tissue, and the body's immune system can mount a delayed attack years or decades later — especially after immune-triggering events like illness or vaccination.

Common Symptoms
Foreign Protein Immune Response
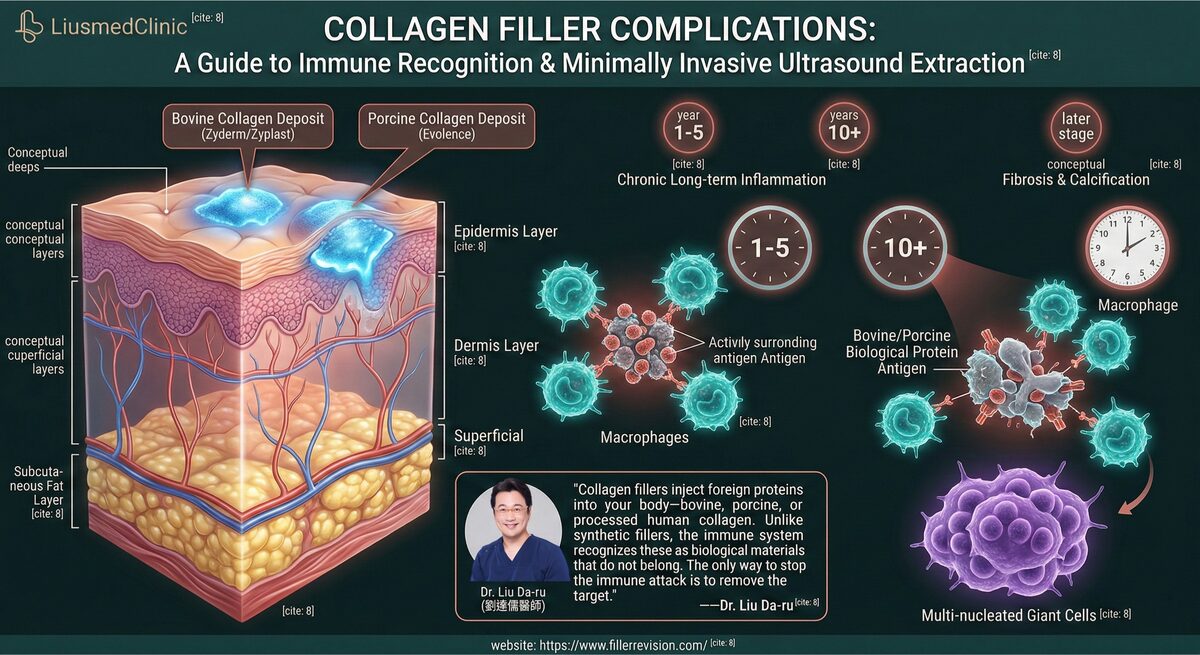
Collagen filler patients who find FILLER REVISION share the same bewilderment: 'How can something from 25 years ago still be causing problems?' The answer lies in the unique biology of these legacy products — and explains why their current doctors, who've never used these fillers, have no idea how to treat the complications. Bovine collagen (Zyderm/Zyplast) contains cow-derived protein that 3-5% of patients develop antibodies against—even after passing pre-treatment skin tests. Porcine collagen (Evolence) similarly triggers immune recognition. The body's immune system identifies these foreign proteins and mounts a sustained inflammatory response: macrophages surround the collagen deposits, attempting to degrade and isolate them. This foreign body response leads to granuloma formation—organized immune cell aggregates that create firm, palpable nodules. Over time, the chronic inflammation stimulates fibrosis and calcification, transforming soft collagen deposits into hard, permanent masses. Even human-derived collagen products (CosmoDerm) can trigger reactions when injected into tissue planes where the processing has altered the protein's native structure.
Why Traditional Treatments Fail
Why Steroids and Dissolution Fail
Standard treatment protocols for collagen filler complications rely on intralesional steroid injections to suppress the immune response and 5-fluorouracil to slow fibroblast activity. While these treatments may temporarily reduce inflammation and swelling, they do not remove the foreign protein that is triggering the immune response. Steroids carry significant risks with repeated use: skin atrophy, telangiectasia, fat atrophy, and depigmentation. The immune system will reactivate once steroid effects wear off, because the antigenic stimulus—the foreign collagen—remains in place. There is no enzyme equivalent to hyaluronidase for collagen fillers; collagenase is not approved for facial soft-tissue use. This leaves patients in a cycle of steroid-suppress-flare-repeat that never achieves resolution.
“At FILLER REVISION, collagen filler patients often arrive after being dismissed by 2-3 modern practitioners who've never even seen these products. 'I had this done in 1998 — how can it still be there?' The body encapsulated it rather than absorbing it, and now an immune trigger has reawakened the response decades later. The irony is that these legacy deposits are some of the most straightforward cases we treat — well-encapsulated, clearly visible on ultrasound, and highly responsive to extraction.”
Dr. LiuRemove the Antigen, Resolve the Reaction
Ultrasound-Guided Pinhole Micro-Extraction
Collagen filler complications are fundamentally immune-mediated — the body recognizes foreign protein and mounts a sustained attack against it. Steroid suppression treats the symptom (inflammation) but not the cause (foreign protein). Definitive resolution requires removing the antigenic material, not suppressing the body's natural defense response.
Your Doctor Has Never Seen This Product — We See It Weekly
At FILLER REVISION, legacy collagen filler cases are a core specialty. Most modern practitioners have never treated Zyderm, Zyplast, or Evolence complications because these products predate their careers. Revision demands both ultrasound imaging and specific experience with how biological fillers behave differently from the HA and synthetic products used today.
The Inflammation Is a Signal, Not the Disease
Steroids suppress your immune system's correct identification of foreign protein — treating the alarm, not the fire. At FILLER REVISION, we remove the antigenic target itself, which is why our results are permanent while steroid relief is always temporary.
25-Year-Old Deposits, One-Session Extraction
The irony of legacy collagen complications is that the very encapsulation that makes them persistent also makes them excellent extraction candidates. Well-defined capsules, clear ultrasound visibility, and predictable tissue planes — FILLER REVISION patients are often surprised at how straightforward the procedure is after decades of being told nothing could be done.
Ultrasound-Guided Micro-Extraction
We directly remove the collagen deposits and their surrounding fibrous capsules through pinhole entries under real-time ultrasound guidance. By physically extracting the foreign protein material, we eliminate the antigenic stimulus driving the immune response—achieving definitive resolution rather than temporary suppression. For calcified deposits, we use specialized techniques to fragment and aspirate the hardened material. The ultrasound allows us to distinguish between active inflammatory tissue, fibrotic capsule, and residual collagen product, enabling precise extraction with minimal disruption to surrounding healthy tissue.
Ultrasound Deposit Mapping
Capsulotomy & Protein Extraction
Calcification Fragmentation
Anti-Inflammatory Irrigation
Before & After Results
View real patient results for this condition, including ultrasound imaging before and after extraction.
View All Case ResultsCommon Questions
Yes. Collagen filler deposits can remain in tissue for decades, particularly when they become encapsulated by fibrous tissue or calcify. The immune system continues to recognize the foreign protein indefinitely, which is why delayed reactions can appear years or even decades after the original injection. Many patients we treat had their injections in the 1990s or 2000s.
When your immune system is activated by illness, vaccination, or stress, the heightened immune response also amplifies the reaction against the foreign collagen protein in your tissue. This cross-activation causes the characteristic flare-up pattern—the deposits swell and become painful during periods of immune stimulation, then partially subside as the acute immune response resolves.
No. There is no FDA-approved enzyme for dissolving collagen fillers in facial soft tissue. Unlike hyaluronic acid, which can be broken down by hyaluronidase, collagen filler deposits must be physically removed. This is why ultrasound-guided extraction is the definitive treatment—it removes the source material rather than attempting chemical dissolution.
Calcified collagen deposits are common in long-standing cases. These hardened masses can be fragmented using specialized needle techniques under ultrasound guidance, then aspirated through pinhole entries. The calcification actually makes the deposits easier to identify on ultrasound, allowing very precise targeting.
Historical data shows that approximately 1-3% of patients who passed the standard double skin test still developed hypersensitivity reactions after injection. The skin test detected only immediate-type reactions, missing delayed-type hypersensitivity that could manifest weeks to months later. This is one reason bovine collagen fillers fell out of favor.
Once the foreign collagen protein is physically extracted, the immune stimulus is eliminated and the inflammatory response resolves permanently. Unlike steroid suppression, which leaves the triggering material in place, extraction is definitive. The granulomatous reaction cannot recur without the antigenic foreign material to sustain it.
Most patients experience mild swelling and tenderness for 3-5 days. Bruising typically resolves within 7-10 days. The inflammatory response begins to subside within days of extraction as the immune system no longer has a foreign protein target to attack. Final contour results are visible at 2-4 weeks.
This is common — collagen fillers haven't been widely used since the mid-2000s, so many current practitioners have no experience with their complications. You need a specialist with both ultrasound imaging capability and experience with legacy filler extraction. This is exactly the type of case our clinic specializes in — we regularly treat complications from products that most modern injectors have never even seen.
Yes — though prolonged steroid use does create additional challenges. At FILLER REVISION, we commonly treat collagen filler patients who've endured years of steroid management. The steroids may have caused local fat atrophy, skin thinning, or telangiectasia around the deposit, but the foreign protein core remains extractable. In fact, ending the steroid cycle is one of the most immediate benefits of extraction — patients are often as relieved to stop the steroids as they are to have the lump removed.
Posted in the forum? We can help expedite your appointment.
Standard booking takes 3+ months. If you post your case in the FillerRescue forum first and then add LINE @liusmed with the required info, we’ll watch for earlier slots and help arrange your appointment as soon as possible.
In your LINE message, mention you posted in the FillerRescue forum.
References
- Lemperle G, et al. Foreign body granulomas after all injectable dermal fillers: part 1. Possible causes. Plast Reconstr Surg. 2009;123(6):1842-1863.
- Duranti F, et al. Injectable hyaluronic acid gel for soft tissue augmentation. A clinical and histological study. Dermatol Surg. 1998;24(12):1317-1325.
- Requena L, et al. Adverse reactions to injectable soft tissue fillers. J Am Acad Dermatol. 2011;65(3):604-616.
The information on this website is for educational purposes only and does not constitute medical advice. Individual results may vary depending on personal conditions; actual outcomes cannot be guaranteed. All medical procedures carry potential risks and complications. Please consult a qualified physician before making any treatment decisions.
Featured Poster

Three rounds of dissolving. The lump is still there.
60% of our patients arrive after repeated failed treatments elsewhere. When dissolvers fail, physical extraction is the only answer.